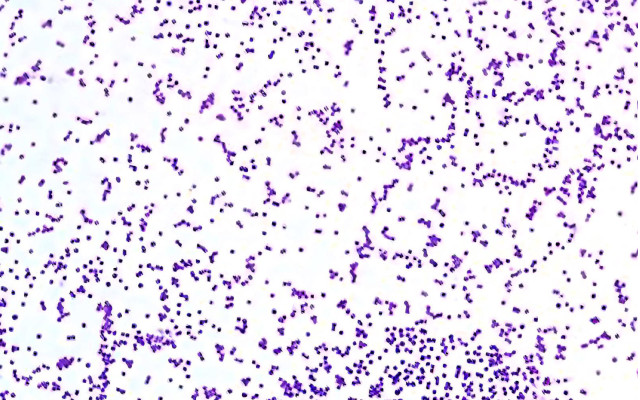
In summer, high temperatures can favor bacterial multiplication in food, especially if kept outside the refrigerator for several hours. This is the case of Staphylococcus aureus, a very common bacterium also on the skin of humans and animals, which can contaminate various food products and cause annoying (although not particularly serious) intoxication.
The bacterium Staphylococcus aureus
S. aureus is a coccal bacterium, Gram positive, immobile, aerobic and facultative anaerobic.
It grows at temperatures between 7 °C and 48,5 °C, with an optimum between 30 °C and 37 °C.
Is responsable of different clinical forms in humans, but the one that results from food contamination is called ‘staphylococcal intoxication’.
Among the numerous jambs that belong to the species, some are in fact capable of producing toxins that have emetic activity, i.e. capable of causing vomiting quickly.
Heat resistant
Staphylococcal toxins (SEs; Staphylococcal Enterotoxins) are small protein chains that are very resistant to heat (therefore, cooking and pasteurization) and UV rays.
Once ingested, are not degraded by the proteolytic enzymes present in the stomach, which they pass through to reach the intestine where they carry out their pathogenic action.
Several variants are known of SEs, of which the SEA, SEB, SEC, SED and SEE are the most studied. However, for symptoms to appear, S. aureus must actively multiply and reach very high values, above 100.000 CFU/gram of food.
In these conditions, the quantity of toxins produced is sufficient to trigger the harmful event in the consumer, which however cannot occur in the presence of a low bacterial load.
Food at risk
Staphylococcus aureus, due to its widespread diffusion on the epidermis, nasal mucosa and scalp of people, can easily transfer to foods during their preparation, if workers do not follow basic hygiene rules, such as wearing gloves and a hat.
Even the animal, in addition to humans, may have an important role in S. aureus contamination; just think of milk, contaminated by cows, sheep and goats affected by staphylococcal mastitis.
Biofilm on tools
Another feature which facilitates the transmission of S. aureus to food is its ability to form biofilms, i.e. bacterial aggregates that adhere to the surface of various equipment (such as knives, containers, blenders, etc.) and spread to products that come into contact with them.
At risk are mainly processed milk-based foods, such as custards, cream and desserts filled with cream, or various delicatessen products, and meat preparations (roasts and skewers of chicken, turkey and beef) kept at temperatures that allow the growth of S. aureus.
The foods most at risk
Meat products not subjected to cooking (such as fresh sausages, minced meat or whole cuts) are not at risk like others, given that Staphylococcus aureus grows more easily in foods with a low microbial load.
This is the case with products of pastry, gastronomy and meat preparations subjected to cooking (with consequent reduction of the bacterial flora, destroyed by heat), contaminated after heat treatment by the hands of operators or by equipment and surfaces not appropriately sanitized.
Habit keeping risky foods at room temperature is strongly discouraged, especially in summer when it gets dangerously close to the optimal temperature, at which S. aureus multiplies rapidly and is able, in a few hours, to reach very high values.
The symptomatology
In the consumer SEs toxins cause nausea and vomiting, defined as incoercible or ‘projectile’ due to its intensity, sometimes accompanied by abdominal pain and diarrhoea.
Weakness and slight increase in temperature bodily symptoms may appear alongside gastro-intestinal symptoms.
Symptoms appear shortly after the meal, normally within 3-5 hours of ingestion of the contaminated product (with extremes of 30 minutes-8 hours), and resolve within 24 hours.
More severe frameworks, especially linked to the danger of dehydration, can appear in very young children and the elderly.
What prevention
To prevent staphylococcal intoxication must be played on two fronts:
- personal and environmental hygiene e
- the correct conservation of risky foods.
People who handle food must take care of their personal hygiene, wear disposable gloves and a hat, apply waterproof plasters on small wounds and pimples (often the site of S. aureus) and correctly sanitize the equipment used in the processing of food products, to reduce the formation of bacterial biofilms.
It is also fundamental separate the storage and preparation areas of raw products from cooked ones, to avoid cross-contamination phenomena. As already mentioned, it is very important to prevent the rapid and excessive development of Staphylococcus aureus by keeping foods at risk at temperatures below 4°C or above 60°C. In both cases, the growth of S. aureus, and the resulting production of toxins, is prevented.
The legislation
The research of Staphylococcus aureus is required by Italian and European legislation on the hygiene of food products.
Particularly, the S. aureus strains that elaborate the coagulase enzyme, which is related to the synthesis of SEs, are the subject of analysis.
EC Regulation 2073/2005 on the microbiological criteria of food products provides for the counting of coagulase-positive S. aureus to evaluate the production hygiene of various types of dairy products (raw milk cheeses or cheeses subjected to heat treatment, unripened soft cheeses, unripened butter and cream pasteurized products, milk and whey powder), while the absence of SEs toxins is required in the same products offered for sale.
Even raw milk, if sold directly from the stable to the final consumer, must be analyzed for S. aureus, as an indicator of milking hygiene (State-Regions Agreement of 25 January 2007).
Silvia Bonardi
REFERENCES
Le Loir Y, Baron F, Gautier M. Staphylococcus aureus and food poisoning. Genet Mol Res. 2003 Mar 31;2(1):63-76. PMID: 12917803.
Abril AG, Villa TG, Barros-Velázquez J, Cañas B, Sánchez-Pérez A, Calo-Mata P, Carrera M. Staphylococcus aureus Exotoxins and Their Detection in the Dairy Industry and Mastitis. Toxins (Basel). 2020 Aug 20;12(9):537. doi: 10.3390/toxins12090537.
Kadariya J, Smith TC, Thapaliya D. Staphylococcus aureus and staphylococcal food-borne disease: an ongoing challenge in public health. Biomed Res Int. 2014; 2014:827965. doi: 10.1155/2014/827965.
Regulation (EC) no. 2073/2005 of the Commission, of 15 November 2005, on microbiological criteria applicable to food products. Official Journal of the European Union L 338 of 22.12.2005, p. 1–26
Graduated in Veterinary Medicine and Specialist in Inspection of Food of Animal Origin and in Veterinary Public Health, she is Professor of Inspection and Control of Food of Animal Origin at the University of Parma.